Hearing Testing

PURE TONE AUDIOMETRY (PTA)
It is a hearing test used for both screening and diagnosis purposes. This test determines not only presence or absence of hearing loss but also type, degree and configuration of hearing loss. Each ear will be tested individually. This information is critical to determine if medical or surgical intervention is possible or if hearing aids may help. This test provides information about which part of the ear problem occurs like the outer ear, middle ear or inner ear and what are possible treatment.

Impedance Audiometry(IA) test
Impedance audiometry (IA) test includes tympanometry and acoustic reflex measurements. Impedance audiometry provides information about eardrum or middle ear disorders such as chronic otitis media with effusion (COME), tympanic membrane perforation, otosclerosis, and others. This information is crucial for the treatment of middle ear disorders.
The Eustachian Tube Function (ETF) test, also performed with the same instrument, provides important information about middle ear problems and Eustachian tube functioning.
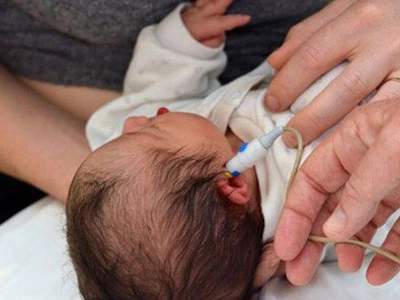
OTO-ACOUSTIC EMISSIONS (OAEs)
OAEs were mostly used as screening test to new born child which assess the functioning of the outer hair cells within the cochlea of the inner ear. This test provides results as Pass or Refer. Pass result indicative of at that time hearing is normal and Refer indicates that child needed further detailed investigation for hearing which is generally done with BERA test. In conjunction with BERA, OAEs are often used to differentially diagnose auditory neuropathy - a disorder of the auditory nerve
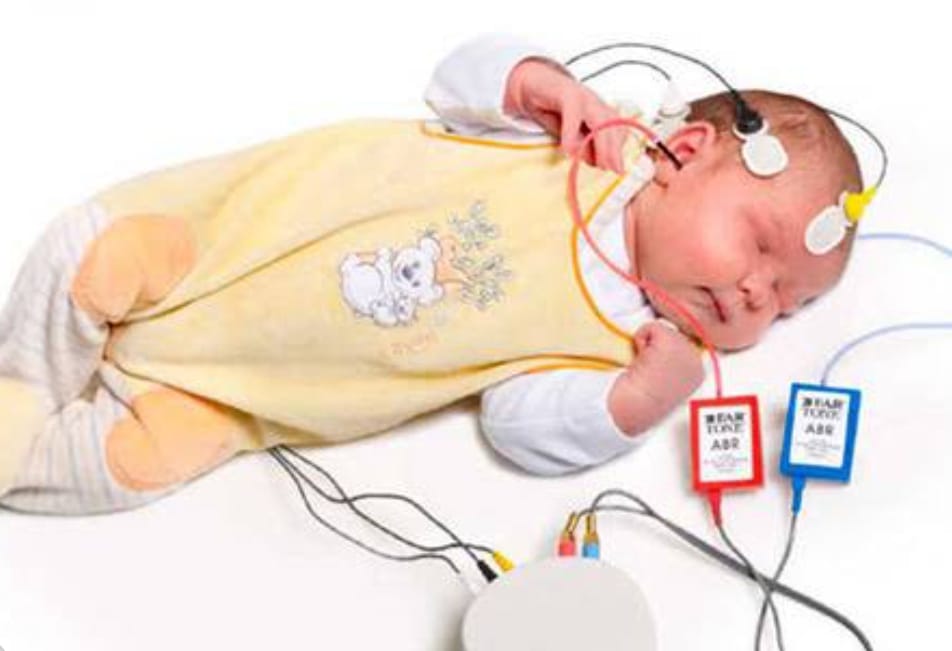
Brainstem Evoked Response Audiometry (BERA ) or Auditory Brainstem Response (ABR) Tests
It is a neurophysiological method used to assess the auditory pathway up to the brainstem. It evaluates the function of the auditory nerve and brainstem in response to sound stimuli. This test is used to diagnose hearing loss, especially in infants and young children who cannot participate in conventional hearing tests as this test do not require the child to respond to the sounds. It also helps to identify the site of lesion in patients with suspected retro-cochlear pathology, such as acoustic neuromas or auditory neuropathy.

Auditory steady state Response (ASSR)
This test is an advanced auditory evoked potential test used to objectively assess hearing thresholds. Unlike traditional auditory tests, ASSR can estimate hearing sensitivity across different frequencies simultaneously and is particularly useful for diagnosing various degrees of hearing loss, including profound hearing loss.
It is used to evaluate hearing thresholds across a wide range of frequencies in individuals who cannot provide reliable behavioral responses, such as infants and those with developmental disabilities.
Cochlear implant NRT and Mapping
Cochlear implants use Neural Response Telemetry (NRT) and mapping to optimize the device’s performance for each user.
Neural Response Telemetry (NRT): - Neural Response Telemetry is a technique used to measure the electrical responses of the auditory nerve to stimulation from the cochlear implant. It helps audiologists and surgeons ensure that the implant's electrodes are correctly positioned and functioning as intended.
Mapping: - Mapping is the process of programming the cochlear implant to suit the specific hearing needs of the user. This involves setting the electrical stimulation levels for each electrode on the implant to ensure optimal hearing performance.
By combining NRT and detailed mapping procedures, audiologists can maximize the benefits of cochlear implants, leading to significant improvements in hearing and quality of life for recipients.

New Born and Industrial Hearing Screening
Newborn hearing screening is a critical procedure to identify hearing loss at an early stage. Early detection is essential for timely intervention, which can significantly improve language, social, and cognitive development. This screening typically involves two primary tests: 1. Otoacoustic Emissions (OAE): and Automated Auditory Brainstem Response (AABR).
Industrial hearing screening is conducted to monitor and protect the hearing of workers exposed to high levels of noise in industrial settings. Regular hearing tests help in early detection of noise-induced hearing loss, ensuring timely protective measures can be implemented.
Both types of screening are vital for preventing and managing hearing loss in their respective populations.

Tinnitus Evaluation and Management
Many individuals experience a persistent buzzing or ringing in their ears, a condition known as tinnitus. Tinnitus can manifest as various sounds, including buzzing, ringing, hissing, pulsatile noises, or whistling.
An audiologist plays a crucial role in evaluating tinnitus. This process typically involves collecting detailed information about the patient's tinnitus, such as its onset, duration, pitch, loudness, and any factors that worsen or alleviate the symptoms. Audiologists also perform Tinnitus Matching to measure the pitch and loudness of the tinnitus, gaining a better understanding of its characteristics.
Based on the evaluation, the audiologist can offer various management strategies, including:
- *Sound Therapy*: Using background sounds to make tinnitus less noticeable.
- *Hearing Aids*: For patients with hearing loss, these can amplify external sounds, reducing the prominence of tinnitus.
- *Masking Devices*: These produce white noise or other soothing sounds to cover the tinnitus.
- *Tinnitus Retraining Therapy (TRT)*: This combines sound therapy with counseling to help patients habituate to the tinnitus.
Through these strategies, audiologists aim to improve the quality of life for individuals affected by tinnitus.
Speech Therapy
Speech therapy is a treatment of speech disorders or communication problems. Speech therapy is a clinical program aimed at improving speech and language skills and oral motor abilities. It is conducted by speech-language pathologists (SLPs), also known as speech therapists.
Speech therapy can be beneficial for individuals of all ages with various conditions, including speech delays, articulation disorders, language disorders, voice disorders, fluency disorders (like stuttering), and cognitive-communication disorders. It can also assist those who have experienced stroke, brain injury, or other conditions affecting communication and swallowing abilities.
Shravya Speech and hearing clinic has one of the best speech therapists team who specialize in diagnosing, evaluating, and treating communication disorders, swallowing disorders, voice disorders, and cognitive-communication disorder. A speech-language pathologist plays a crucial role in the treatment of autism spectrum disorder
Speech therapists are educated to identify the problem and disorder and find the best way to treat it. The speech therapists study human communication, development in human communication, and its disorders.
A speech therapist must have the required qualification/degree like BASLP/MASLP or DHLS for assistance
The SPL should have a license/ certification in this field which is provided by Rehabilitation Counsel of India (RCI)
The speech therapists of Shravya Clinic work one-and-one with every child to help them to overcome their problems. They treat children or adults with Hearing impairments, Autism Spectrum Disorder, Down. Syndrome, Stuttering/stammering, Misarticulation, Neurological Speech or language disorders..etc .
It is better if the therapy starts as early as possible. Children below 5 learn better than those who begin later. This doesn’t mean that children who start therapy later in life don’t show effective results. They learn a little slower as they have learned patterns that need to be changed during therapy.
It is better to start therapy as early as possible. A child may need speech therapy if they exhibit difficulties in any of the following areas:
1. *Speech Delays:* If a child is not meeting speech and language milestones for their age, such as not babbling by 12 months, not speaking any words by 18 months, or having fewer than 50 words by age 2.
2. *Speech Sound Disorders:* Difficulty pronouncing sounds correctly, making it hard for others to understand the child. This includes issues like substituting one sound for another (e.g., saying “wabbit” for “rabbit”) or omitting sounds (e.g., saying “nana” for “banana”).
3. *Language Disorders:* Challenges in understanding what others say (receptive language) or expressing thoughts (expressive language). This might include a limited vocabulary, incorrect sentence structure, or trouble following directions.
4. *Stuttering:* Repeating sounds, syllables, or words, prolonging sounds, or having noticeable pauses or blocks when speaking.
5. *Voice Disorders:* Problems with pitch, volume, or quality of the voice that distract listeners or cause the child discomfort.
6. *Social Communication Disorders:* Difficulty with the social aspects of communication, such as maintaining eye contact, understanding and using appropriate gestures, or taking turns in conversation.
7. *Swallowing and Feeding Disorders:* Issues with chewing, swallowing, or feeding that might be related to speech development.
If you suspect a child might need speech therapy, it’s essential to consult our shravya clinic for a comprehensive evaluation.
During speech therapy, various activities and techniques are used to address the specific speech and language needs of the child. Here’s an overview of what typically happens during speech therapy sessions:
### Initial Assessment
1. *Evaluation:*
– The speech-language pathologist (SLP) conducts a comprehensive assessment of the child’s speech, language, and communication skills.
– The assessment may include standardized tests, observations, and parental input.
2. *Diagnosis and Goal Setting:*
– Based on the assessment, the SLP identifies specific areas of need and sets measurable goals.
– A personalized treatment plan is developed, tailored to the child’s unique requirements.
### Therapy Sessions
1. *Structured Activities:*
– *Articulation Therapy:* Exercises to correct the pronunciation of sounds and improve clarity. This may include modeling correct sounds, practicing with flashcards, and engaging in games that emphasize specific sounds.
– *Language Intervention:* Activities to build vocabulary, sentence structure, and comprehension skills. This might involve storytelling, playing with toys that encourage conversation, and using pictures to stimulate discussion.
2. *Interactive and Play-Based Learning:*
– Incorporating play into therapy to make learning engaging and enjoyable. This can include role-playing, using puppets, and interactive games.
– Using everyday activities and routines to teach language skills naturally.
3. *Pragmatic/Social Skills Training:*
– Exercises to improve social communication, such as making eye contact, taking turns in conversation, and understanding nonverbal cues.
– Practicing appropriate responses in various social situations.
4. *Voice Therapy:*
– Techniques to address voice disorders, including exercises to improve pitch, volume, and quality.
– Breathing exercises and vocal hygiene education.
5. *Fluency Therapy:*
– Techniques to manage stuttering, such as slow speech practice, controlled breathing, and gradual exposure to speaking in different situations.
6. *Augmentative and Alternative Communication (AAC):*
– For children with severe communication challenges, using tools like picture boards, sign language, or speech-generating devices to facilitate communication.
### Parental Involvement
1. *Home Practice:*
– The SLP provides exercises and activities for parents to practice with the child at home, reinforcing therapy goals.
– Guidance on how to integrate speech and language practice into daily routines.
2. *Progress Updates:*
– Regular communication between the SLP and parents to discuss the child’s progress and any adjustments needed in the therapy plan.
### Monitoring and Adjusting
1. *Ongoing Assessment:*
– Continuous monitoring of the child’s progress toward therapy goals.
– Adjusting the therapy plan as needed based on the child’s development and response to therapy.
2. *Graduation from Therapy:*
– When the child achieves their speech and language goals, the SLP will gradually reduce the frequency of sessions and eventually discharge the child from therapy, while providing strategies to maintain progress.
Overall, speech therapy is a dynamic and interactive process tailored to each child’s specific needs, aiming to improve their communication skills and enhance their ability to interact effectively with others.
1. Delayed Speech and Language Development (DSL)
2. Hearing impairment (HI)
3. Autism Spectrum Disorder (ASD)
4. Mental Retardation(MR)
5. Down syndrome
6. Stuttering/Stammering
7. Misarticulation
8. Voice Disorders
9. Dyslexia and Reading Disorders
10. Auditory Processing Disorders
11. Feeding and Swallowing Disorders (Dysphagia)
12. Neurological Speech or language disorders(Aphasia, dysarthria..etc)
Speech therapy offers numerous benefits for individuals with communication and swallowing disorders. Some of the key benefits include:
1. *Improved Communication*: Enhances the ability to express thoughts and ideas clearly, both verbally and non-verbally.
2. *Enhanced Language Skills*: Helps in developing better understanding and use of language, both spoken and written.
3. *Better Articulation and Pronunciation*: Improves the clarity of speech, making it easier for others to understand.
4. *Fluency Improvement*: Reduces stuttering and other fluency disorders, leading to more fluid and natural speech.
5. *Stronger Voice*: Addresses issues with pitch, volume, and quality of voice, leading to healthier and more effective vocal use.
6. *Swallowing Safety*: Assists in managing and treating dysphagia, reducing the risk of choking and aspiration, and improving overall swallowing function.
7. *Enhanced Cognitive-Communication*: Supports individuals with cognitive impairments in improving their memory, attention, and problem-solving skills related to communication.
8. *Improved Social Communication*: Helps individuals develop better social interaction skills, such as understanding social cues, turn-taking, and maintaining eye contact.
9. *Increased Confidence and Self-Esteem*: As communication skills improve, individuals often experience a boost in confidence and self-esteem.
10. *Academic and Professional Success*: Enhances performance in school or work settings by improving communication and comprehension skills.
11. *Better Quality of Life*: Overall improvement in communication abilities leads to more effective interactions and participation in daily activities, enhancing the quality of life.
Speech therapy is tailored to each individual’s needs, making it a highly personalized form of treatment that can address a wide range of issues and provide substantial benefits across different areas of life.
1. Speech Assessment
2. Speech Language Therapy
3. Applied Behavioral Analysis(ABA) therapy
4. Sensory Integration Therapy (SIT)
5. Cognitive Behavioral Therapy (CBT)
6. Social Skills Training (SST)
7. Occupational Therapy
8. Special Education
9. Auditory Training
10. Auditory Verbal Therapy (AVT)
9. Swallowing Therapy
10. Voice Therapy
11. Articulation therapy
12. Fluency therapy
